BREAST CENTER & BREAST CLINIC
REA Breast Center & Breast Clinic features latest technology equipment and all doctors are specialized in breast disease treatments.
REA Breast Clinic with full diagnostic equipment for diagnosis of any type of condition, either benign or malignant, features the following:
- Offices for breast surgeons-mastologists, specialized abroad in full breast examination and breast ultrasounds. Capacity for cytological examination of nipple discharge (mammary pump) and fine needle aspiration (FNA).
- Imaging department for 3D ultrasound scans, super sonic elastography for diagnosis of any benign and malignant breast conditions and assisted biopsy. The department features two high-tech, high resolution mammography units with tomosynthesis option (only 2 in Greece) allowing a full and detailed diagnosis of premalignant and early-stage lesions.
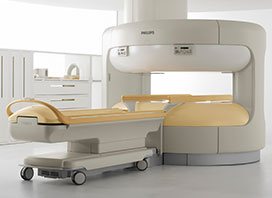
- Specialized radiologists with magnified spot view and stereotactic biopsy (mammotome) eliminate pseudo-negative results. The imaging department is also equipped with a CT and MRI scanner (Breast MRI) with specialized scientific personnel. Such scans may be performed as additional to mammography, in special cases of women in high risk and in differential diagnosis of small atypical nodules, but also to follow-up women that have undergone a surgery for breast cancer.
- Microbiology laboratory for special exams of breast conditions, cancer markers with CA15-3 and a new more sensitive CA27-29. Gene control for cases with hereditary breast and ovary cancer with BRCA1, BRCA2 detection.
- Pathological-anatomical laboratory for a rapid biopsy, examination of oncogens and hormone receptors.
- Cytology laboratory for Breast PAP test with a double technique of GIEMSA smear and PAP smear, liquid-based cytology (Breast ThinPrep) and nipple Duct lavage, the only one in Greece.
Linked to REA Breast Center, in case of a breast surgery in REA Hospital, breast surgeons apply the most updated techniques in breast surgery:
- Microbiopsies
- Macrobiopsies
- Ductoscopy
- Sentinel lymph node (SLN) biopsy (stain, radioactive), avoiding complications in lymph nodes removal in cases of breast cancer.
- Pyramidectomy or microdochectomy, surgery for breast duct excision in case of pathological discharge or microbiological lump.
- Oncoplastic surgeries, combining surgical oncology with aesthetic surgery.
Additionally, oncology meetings and special meetings are organized after breast Ca by a team of experts and university doctors of our Clinic.
Mammography
Breast cancer is the most common neoplasm in women and it is the second cause of cancer death after lung cancer. Each year in the USA, 180,000 new cases of breast cancer are diagnosed and about 40,000 women die of the disease. Both in USA and Europe, from 1940 to 1980 there was an increase in the incidence of breast cancer. Genetic factors have been accused as a main cause of breast cancer, but environmental factors should also be considered.
For example, women that migrated from regions with a low incidence of breast cancer (e.g. Japan) to regions with a high incidence (e.g. USA) have shown an increase in the risk of developing breast cancer that also increases for every younger generation. It is though comforting the fact the in recent years there is a reduction of deaths caused by breast cancer. This is due to generalized monitoring procedures with mammography and evolution in chemotherapy and radiotherapy. Breast cancer occurs in 5% of women under 40 years old, 20% of women between the age of 40 and 50 and 75% of women between 50 and 70 years old.
Apart from the age, various genetic factors may also cause 5% of breast cancer cases. The discovery of the BRCA-1 and BRCA-2 genes has indicated that a part of the population is in higher risk of developing breast cancer. In addition, women with family history of breast cancer in their mother’s family (especially in case of premenopausal breast cancer) have an increased risk of developing breast cancer themselves.
Other increased risk factors, except for genetic factors, include:
- female infertility
- first childbirth after the age of 30
- premature menstruation
- delayed menopause
- taking hormones for a premature menopause
- hormone therapy (estrogens, contraceptive pills, IVF)
- obesity
- lack of breastfeeding
- history of breast cancer, etc.
Breast cancer prevention is a very important factor for every woman. Mammography may result to a 30% reduction of breast cancer deaths, especially for women between 50 and 70 years old.
There are certain disputes among countries on the age that a mammography screening should be performed for the first time and on the frequency, it should be repeated. In several countries, like USA, the following are recommended:
- Annual mammography or every 2 years maximum for women at the age of 40-45 years.
- Annual mammography for women of 50-70 years old.
- Repeat mammography screening every 2 years for women over 70 years old.
- First mammography at the age of 35 for women with family history of breast cancer
- First mammography at the age of 25 for women with possible family history and BRCA 1 or 2
- Mammography for women with suspicious nodules, discharge or swelling of breast skin
A common question is whether mammography radiation may cause problems or even breast cancer. It has to be noted that radiation absorption is really low (less than 1 rad). In general, with today’s technology, there is practically no such risk for women over 40 years of age. There may be a slight risk for women under 20 years or between 20 and 30 years. It has to be understood that digital mammography, apart from better detection, transmits far less radiation compared with classic analogue mammography.
Finally, we need to mention that as in any examination, there is a low false-positive rate in mammography as well. However, digital mammography conducted by well-experienced radiologists for better imaging greatly reduces the above rates.
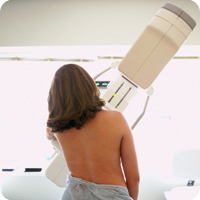
Mammography is an x-ray examination of the breast. It is used to detect and evaluate breast diseases, both in women who have no breast complaints or symptoms and in women who have breast findings or symptoms, such as palpable findings, pain or nipple discharge.
Digital mammography is a newer method for breast x-ray with less radiation and higher definition, compared to old analogue mammograms. In REA Breast Center, digital mammography uses the new CAD system, detecting suspicious areas in mammograms that need further checking.
There are two types of mammographic examinations: screening mammography and diagnostic mammography.
Screening Mammography
Screening mammography is an examination used to detect early breast cancer in women with no symptoms. A mammogram is really important for a timely breast cancer diagnosis, as it can show changes in density of breast parenchyma or other findings, up to two years before the patient or treating physician may be able to clinically detect it.
Screening mammography is indicated by the age of 35 and then every year from the age of 40. Women that had breast cancer or are in a high-risk group (family history, positive genetic testing) must consult their treating physician or a mastologist. They may need to start with screening checks before the age of 35 or increase the frequency of screening tests.
Diagnostic Mammography (Detection mammography or breast tomosynthesis)
Diagnostic mammography is used to evaluate a patient with pathological clinical findings, such as palpable findings (breast lumps), nipple discharge, nipple eczema, etc. Diagnostic mammography (detection mammography or breast tomosynthesis) is also performed to patients that have shown suspicious changes in their screening mammography.
During all x-ray tests, special precautions are taken in order to use the lowest radiation dose possible while producing the best possible images for screening and evaluation. All national and international organization guidelines on radiation protection are followed.
Our state-of-the-art equipment provides a better focus of used radiation to ensure the least possible use of it. During mammography testing, transmitted radiation is not enough to reach the uterus; however, we do still prefer to avoid routine mammograms to women that may be pregnant. For urgent breast problems, consult the mammography technologist in order to find the best and safest way of problem evaluation.
Preparation for your mammography
It would be better before proceeding with a mammogram to discuss with your treating physician about any new findings in your breast, any previous surgeries, any use of hormones and your family or personal history for breast cancer.
What to wear
On the day of the examination, avoid using deodorants, antiperspirants, any powder or cream, as certain of their constituents can appear on the scan and cause confusion over the diagnosis. Since you will need to undress from the waist up, you are advised to avoid one-piece outfits. Before the screening, you will be asked for your medical history that is related to your breast pathology.
Examination
The technologist will take you to the examination room, where you will be asked to undress from your waist up and you will be given a hospital gown. The technologist that will perform your examination is a highly trained person in breast diseases and can respond to any questions you may have.
During the screening process, you will feel pressure on your breasts. Some women with sensitive breasts may experience some discomfort. This is why mammography should be scheduled after your period has finished when your breast is less sensitive. Pressure has to be placed on your breasts in order to:
- even out the breast thickness so that all of the tissue can be visualized
- spread out the tissue so that small abnormalities are less likely to be obscured by overlying breast tissue
- allow the use of a lower x-ray dose since a thinner amount of breast tissue is being imaged
- hold the breast still in order to minimize blurring of the image caused by motion.