UROLOGY DEPARTMENT

REA Hospital’s Urology Clinic offers a comprehensive approach to urinary tract diseases that follows high medical standards.
REA Hospital’s experienced team of urologists, specially trained in the contemporary techniques of°diagnosing and treating urologic conditions, combined with the°latest-generation equipment that is provided, guarantee the expert treatment and quick recovery of our patients.
Our aim is to offer high quality care, from the first visit and diagnosis, to the invasive treatment of the condition and the subsequent monitoring.
Meet REA’s Urology Clinic
Our specialisation in the whole range of urological conditions, as well as in all malignancies of the urinary system, offers individualised monitoring throughout the course of the patient's hospitalisation. Through the use of the most contemporary°and°innovative equipment, we aim °to optimise the accuracy of diagnosis,°safety in°treatment,°patient comfort°and °rapid recovery.
Indicatively, the center supports 3D Laparoscopic Surgery in high-definition (4K) monitors,°laser°treatments with high-energy equipment, as well as a full range of endourological procedures with latest-generation endoscopes.
All advanced methods of minimally invasive urology are applied, ensuring°excellent surgical°results and°faster recovery°for the patient. Most patients undergoing even the most severe oncological and endourological procedures are discharged on the first postoperative day and return to their daily activities very soon.
Also, the urology team of REA is supported by a large team of different surgical and pathological specialties, in order to deal with even the most complex cases. Specifically, in cases of malignancy treatment, the oncology board of the clinic advises the optimal protocol of treatment to be followed by doctors of other specialties (oncologists, radiation therapists, etc.). In this way, the entire "course" of the patient is controlled in its different stages, from the diagnosis and treatment, to the subsequent monitoring and counseling.
The conditions that are treated fall into the following categories:
UROLOGICAL ONCOLOGY
The Urology department of the REA Hospital places special emphasis on treating diseases such as kidney cancer, prostate cancer, bladder cancer, testicular cancer and penile cancer by applying the most modern and safe techniques for each disease.
Kidney Cancer
What is kidney cancer?
The kidneys are two organs located on the sides of the spine and are involved in many functions of the human body, such as regulating blood pressure and filtering blood. Kidney cancer is a°group of tumors of this organ, characterised by the increased and uncontrollable proliferation of malignant cells. These types of cancer are highly heterogeneous in size, form (compact or cystic formations) and histological classification.
How common is it?
Kidney cancer is relatively rare, accounting for 2% of all diagnoses of malignancy worldwide. However, the widespread use of imaging methods (ultrasound, CT scan) has led to the detection of more tumors found accidentally at an earlier stage, thus increasing the survival rates of the disease. The disease occurs more often in men than in women, with the average age of diagnosis being°between 60 and 70 years of age.
What are the symptoms of kidney cancer?
In most cases, kidney cancer is°asymptomatic°and is discovered accidentally in an imaging procedure performed on different medical grounds. About 1 in 10 patients may experience symptoms such as back or side abdominal pain, a palpable abdominal mass or blood in their urine. More rarely, various agents released from the tumor into the bloodstream can lead to systemic effects, such as anemia, hypertension or fever (paraneoplastic syndrome).
In°cases where the cancer has spread, there may be symptoms in other parts of the body, such as bone pain or persistent cough.
How is it diagnosed?
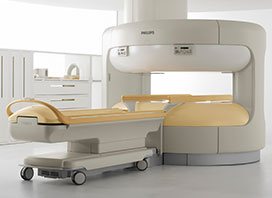
The diagnosis is made by imaging methods, such as ultrasound (U/S), CT and/or MRI scan (C/T – MRI).
How is kidney cancer treated?
The surgical treatment of renal cancer in REA Hospital is carried out through laparoscopy or open access, always depending on the history and particularities of each patient and within the context of their individualised approach.
In cases of partial nephrectomy, which is always performed with a view to maintaining the highest possible rate of healthy renal parenchyma, our Clinic applies the technique of ‘’clampless partial nephrectomy’’ or ‘’selective clamping’’, where appropriate, optimising the maintenance of renal function, especially in cases of patients with only one kidney and/or impaired renal function.
Prostate Cancer
What is prostate cancer?
Like any structure in the human body, the prostate gland is made up of cells. The abnormal and uncontrolled proliferation of these cells, for unknown reasons, is prostate cancer. Prostate cancer is the most common type of cancer found in men and the second most common type of cancer that causes mortality in men, after lung cancer. As with most cancers, the exact causes are unclear. Prostate cancer is considered a multifactorial condition, which is caused by both hereditary and environmental parameters, as well as lifestyle.
Who is at increased risk for prostate cancer?
The exact reason for developing prostate cancer is not yet known; specific factors have been associated with an increased incidence of prostate cancer. The risk factors are:
- Age: the most important risk factor for prostate cancer. In Europe, prostate cancer is usually diagnosed in people over the age of 65. However, younger men can also be diagnosed with prostate cancer.
- Ethnicity:African-American men are twice as likely to be diagnosed with prostate cancer as white men. In contrast, Asian descent has been associated with a lower incidence of prostate cancer. The exact reasons for this variation are not known.
- Family history:In men who have first-degree relatives (father, brother, son) diagnosed with prostate cancer, the incidence of prostate cancer is higher.
How is prostate cancer diagnosed?
- By measuring the levels of prostate-specific antigen (PSA) in the blood.
- Digital rectal examination.
- Multiparametric MRI (mpMRI).
- Prostate biopsy.
- Bone scanning/CT scan/PSMA PET-CT scan.
How is prostate cancer treated?
Prostate cancer, in the case of localised disease, can be treated by removing the prostate through radical prostatectomy.
Radical prostatectomy is the surgery to treat prostate cancer, in which the prostate gland is removed radically, that is, along with its capsule and seminal vesicles. The operation is performed by creating a very small incision in the skin and using special laparoscopic instruments, thus minimising surgical trauma to the abdominal wall, postoperative pain and the duration of the patient’s hospitalisation.
Bladder Cancer
What is bladder cancer?
Cancer of the bladder, the organ of the body responsible for the reception, storage and discharge of urine, is a major problem with remarkable medical and social implications.
How common is bladder cancer?
This type of cancer is the tenth most frequently diagnosed cancer in the world.
What causes bladder cancer?
The most important predisposing factor to bladder cancer is smoking, which is responsible for almost half of the cases of malignancy. Also, in the context of their profession, many people are exposed to chemicals such as aromatic amines, aromatic hydrocarbons and chlorinated hydrocarbons, which contribute to the occurrence of about 10% of bladder cancer cases.
What are the symptoms of bladder cancer?
The most common finding in bladder cancer is painless hematuria, which is the presence of blood in the urine. All cases of painless hematuria, microscopic or macroscopic, are considered bladder cancer until proven otherwise. There are patients who may also experience symptoms in the lower urinary tract, such as feeling compelled to urinate, showing increased urinary frequency or even experiencing urinary incontinence. These symptoms, which can occur in other urological conditions, can also occur in a particular type of bladder cancer called carcinoma in situ (in situ carcinoma-CIS).
What tests should I undergo if I have bladder cancer?
If someone develops symptoms that create suspicions of bladder cancer,°the first thing to do is visit an urologist immediately.
In the initial examination of a patient with suspected bladder cancer, CT urography (a CT scan with a focus on the urinary system) and ultrasound of the bladder are some useful imaging tests. These tests allow us to determine the presence of tumors in the urinary tract.
Another method, which sometimes helps us to identify a malignancy in the bladder, is the cytological analysis of urine. This test practically studies the presence of cancer cells in the patient’s urine, which can guide us in diagnosing°cancer in the discharge system of the urinary tract. The cytological analysis of urine contributes mainly to the diagnosis of tumors that are at a higher stage of malignancy, as well as the particular type of cancer mentioned before, CIS.
Also, another test that should be performed on every patient with symptoms of bladder cancer is cystoscopy.
How is bladder cancer treated?
The treatment of bladder cancer depends on the stage of the disease and is usually surgical, combined with chemotherapy and/or immunotherapy and/or radiotherapy.
Surgical treatment,depending on the stage of the disease, may involve either transurethral resection of the tumor or radical cystectomy.
Testicular cancer
What is testicular cancer?
Almost all types of testicular cancer come from the germ cells, the cells involved in the production of sperm.
There are two main categories of testicular cancer, depending on the type of cells:
- Seminomatous tumors: They can develop at any age and are less aggressive.
- Non-seminomatous tumors: They occur more often in younger men, growing and spreading rapidly.
How common is testicular cancer?
Testicular cancer is relatively rare, accounting for 1-1.5% of all cases of cancer in men, but it is the most common type of cancer in men aged 15-35 years.
Are there any risk factors for developing testicular cancer?
- A history of cryptorchidism (a condition in which the testicles do not descend from the abdomen to take their normal position inside the scrotum, the skin that surrounds the testicles).
- Abnormal testicular development.
- Family medical history.
- Presence of cancer in the other testicle.
Is there a way to prevent testicular cancer?
There is no way to prevent testicular cancer, but it is possible to diagnose it at an early stage and this is possible with regular°self-examination, which should take place once a month, every month after puberty. The testicles are superficial organs and their examination/palpation is easy. Through self-examination, everyone can identify by themselves any changes in the shape, size or morphology of the testicles.
What are the symptoms of testicular cancer?
Testicular cancer is usually discovered accidentally by the patient himself, in the form of a painless induration on the testicle. There may (rarely) be swelling and pain, but°testicular cancer is usually painless°and does not show°any symptoms.
In the rare cases where the cancer has spread, there may be symptoms in other parts of the body, such as back or abdominal pain.
How is it diagnosed?
After an induration has been detected by the physician during the clinical examination, further laboratory and imaging testing is recommended:
- Ultrasound: This imaging test can determine the location and texture of the tumor and clarify whether the hardness is due to something compact, such as cancer, or some other benign mass, such as a cyst.
- Blood tests: Tumor markers are substances that occur naturally in the blood, but increase in certain conditions, such as testicular cancer. These markers are detected by a simple blood test. The increase of one or more markers helps to confirm the presence of testicular cancer, but even a negative result does not exclude the presence of cancer.
If the presence of testicular cancer is confirmed,°a CT scan of the abdomen and/or chest is recommended°to assess whether the cancer has spread to lymph nodes in the abdomen or to other areas of the body, such as the lungs.
This process is called°staging°and it will determine the type of therapeutic approach for each patient.
How is testicular cancer treated?
Surgery to remove the°testicle°(radical orchiectomy) is the main first line of treatment for all stages and types°of testicular cancer. During surgery, the surgeon makes an incision in the groin and through this opening extracts the entire testicle. In our clinic, we offer the possibility of partial orchiectomy depending on the stage of the disease and the specific characteristics of each patient (monorchid patient, bilateral tumors, etc.). Then, the patient will be referred to the Oncologist or Radiation therapist for further treatment (if required), always in close contact and cooperation with the attending Urologist.
Penile Cancer
What is penile cancer?
Penile cancer occurs on the skin of the penis or inside the penis. There are several types of penile cancer, depending on the type of cells from which the cancer developed. Squamous cell carcinoma accounts for over 95% of cases of penile cancer. A particular type of squamous cell cancer is carcinoma°in°situ°(CIS), where only skin cells are affected, without the cancer further spreading to the tissue.
How common is penile cancer?
Penile cancer is rare and affects about 1/100,000 men in Europe and the United States. It is more common in men over 60 years of age, but it can also occur at younger ages.
Are there any risk factors for developing penile cancer?
- Phimosis (a condition in which the foreskin, the part of the skin that covers the glans, is narrow or closed and cannot be pulled back to fully reveal the glans)
- Chronic inflammation of the penis such as in recurrent balanoposthitis.
- Scleroatrophic lichen.
- Human Papillomavirus (HPV) infection.
- Treatment of skin diseases with PUVA phototherapy, history of chemotherapy.
What are the symptoms of penile cancer?
Penile cancer usually manifests as some kind of lesion of the skin of the penis. It can occur anywhere on the penis, but occurs more frequently in the glans and foreskin. This lesion can be a rash or, more often, an ulcer. There may be bleeding, itching, a burning sensation or an unpleasant odour.
In the early stages, the penile cancer lesions are usually°painless and many patients do not seek medical attention in time. As a general rule, any change that does not improve within 4 weeks or deteriorates should be checked by a physician.
At a more advanced stage, the patient may notice swelling of the lymph nodes in the groin, experience fatigue, weight loss, abdominal pain and bone pain.
How is it diagnosed?
Medical history and clinical examination are essential. If a suspicious lesion is located on the penis, it is usually followed up by a biopsy, i.e. a small sample of tissue is sent to be examined for cancer cells in the laboratory.
The doctor may also recommend an ultrasound, CT°or°MRI°scan to check the spread of the cancer to the penis, as well as to lymph nodes or other parts of the body. Based on the results of the diagnostic tests, the stage of the cancer is determined. This staging of the disease is what will determine the type of therapeutic approach for each patient.
How is penile cancer treated?
The treatment for penile cancer depends on the size of the affected area and the rate at which the cancer spreads.
More specifically, if the penile cancer is in its early stages, treatment may include: topical use of chemotherapy cream, cryotherapy (which cools and destroys the tissue containing cancer), or laser surgery to remove the affected area, which is usually on the skin.
The main types of treatment for advanced penile cancer are: surgery, radiotherapy and chemotherapy.
Surgery is performed for the most serious lesions, where part of the penis is removed (partial penectomy) or even the entire penis (total penectomy). The operation is combined with radiation therapy and chemotherapy to treat the disease more effectively.
In most cases, any physical changes in the penis after surgery can be corrected with reconstructive plastic surgery.
Total glans resurfacing should be considered as an option for the treatment of all local penile cancers.
If the cancer is diagnosed in time and with the application of contemporary surgical techniques, an experienced urologist is usually able to maintain as much tissue in the penis as possible.
Lymph node cleaning
The treatment for penile cancer often involves inguinal lymph node cleaning, i.e. the surgical removal of the neighboring lymph nodes of the groin, in case the cancer has spread to them.
BENIGN PROSTATIC HYPERPLASIA
Benign prostatic hyperplasia is the enlargement of the prostate, which can cause problems with urination
Learn More
It is a benign condition and occurs after the age of 50, with an increasing frequency as a man ages. Benign prostatic hyperplasia can lead to an increase in PSA, an indicator used for the early diagnosis of prostate cancer, but it is not associated with a risk of urinary neoplasia.
How°is benign prostatic hyperplasia treated?
Depending on the indications that concern the profile of each patient, benign prostatic hyperplasia is treated either pharmaceutically or surgically. On specific indications, transurethral prostatectomy remains the gold standard in the treatment of the symptoms and complications of benign prostatic hyperplasia. In REA Hospital, apart from the standard transurethral prostatectomy, we also offer transurethral bipolar enucleation of the prostate.
URINARY TRACT LITHIASIS
Lithiasis is the formation of kidney stones (nephrolithiasis), which can also occur in the ureters (ureterolithiasis).
Learn More
Acute renal colic is one of the most painful events that one can suffer, and over 50% of patients with colic will relapse in the next five years.
This is a very common condition, since:
One in ten people will develop kidney stones during their lifetime, and this percentage doubles to 20% if there is another member of their family with a history of stone formation.
In recent years, the number of people with kidney stones has doubled, and worldwide it is estimated that 1.2 million people will develop renal colic annually.
How is urinary tract lithiasis treated?
Maintenance treatment
- Treatment of colic with an analgesic regime (medical expulsive therapy).
- Contemporary imaging tests (spiral CT, USNOK, etc.).
- Complete metabolic examination with specialised blood and urine tests, as well as a chemical analysis of the stone.
- Medication for the existing stones and medication aiming to avoid the formation of new ones.
Surgical treatment
Breakdown and removal of kidney or ureteral stones with contemporary, bloodless and painless therapeutic methods, using state-of-the-art machinery and equipment. Urotetroscopy using laser lithotripsy is the most contemporary and safe method of eliminating stones. In our clinic, we offer flexible ureteroscopy-laser lithotripsy.
It is also possible to treat larger kidney stones as well as complicated cases of nephrolithiasis, as there is also a percutaneous nephrolithotomy department (PCNL).
ANDROLOGY
Erectile dysfunction
The possibility to restore erectile function at any degree of the disorder is offered, though maintenance, pharmaceutical or surgical approaches.
Learn More
It is also possible to treat premature ejaculation.
In addition, andrological surgeries of all kinds are performed, such as penile straightening in cases of Peyronie’s disease, phalloplasty, etc.
Fertility problems
It is possible to diagnose and treat infertility in men either by pharmaceutical or surgical means, such as a testicular and sperm biopsy for IVF and/or with the aim of freezing. We always stay in collaboration with the REA Hospital Fertility & IVF Unit, our goal always being to bring children into the world.
RECONSTRUCTIVE UROLOGY
Repair of urinary injury in adults. Repair of congenital abnormalities in the urinary system, as well as iatrogenic lesions.
INCONTINENCE – NEUROUROLOGY – URODYNAMIC TESTING
Rehabilitation of all types of incontinence (urge incontinence, stress incontinence, mixed incontinence) either with maintenance treatment, or with surgical treatment, or a combination of the two, always depending on the indications for each patient.
Learn More
Incontinence is a medical and social issue that concerns both men and women. Urinary incontinence is the involuntary discharge of urine, that is, when we lose urine without wanting to. It is an unpleasant condition, which mainly concerns women after menopause, but also younger women and men, especially after surgery for prostate cancer (e.g. after radical prostatectomy).
Urinary incontinence significantly affects the quality of life of the afflicted individuals, even leading to social withdrawal and depression. For this reason, it is important to know that urinary incontinence is not a normal phenomenon in any case and should be treated with the help of a urologist.
REA Hospital’s Urology Clinic offers the opportunity to proceed with a thorough study and documented diagnosis of these issues with objective criteria (urodynamic testing) when indicated. After the urodynamic test and the evaluation of its results, the treatment of incontinence is approached in the most scientific and personalised way possible.
DEPARTMENT OF MICROSURGERY AND ENDOSCOPY (Short-stay clinic)
The department performs daily flexible cystoscopies, prostate biopsies, as well as operations such as circumcision, cauterisation of warts, reconstructive plastic surgery of the short frenulum, meatotomy and urethral dilation.